TPLO Closure Is a Phase — Not a Moment
Increasingly, surgeons are formalizing how TPLO closure is executed.
Closure marks the transition from surgical control to biological healing.
In TPLO surgery — where implants, exposure, and recovery demands are the norm — how closure is handled matters.
Standardized closure protocols are emerging to reduce variability at the final controllable phase of surgery.

Closure Is the Final Point Under Direct Surgical Control
By the time skin is closed in a TPLO procedure:
- Implants are placed
- Tissue has been exposed
- The operative field is no longer accessible
Decisions made at closure define the handoff from surgical execution to biological healing.
Unlike prep, implants, or antibiotics — which are protocolized — closure has historically been treated as a moment, not a phase. Standardization makes consistency possible.
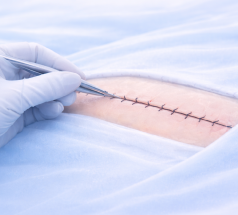
Why TPLO Is Often the First Procedure to Be Standardized
TPLO surgery combines:
- High procedural frequency
- Routine implant placement
- Prolonged exposure
- High functional demand during recovery
For many surgeons, this makes TPLO the natural starting point for defining a consistent closure protocol — one that fits seamlessly into existing workflows without changing technique.
What Surgeons Are Standardizing at Closure
While techniques vary, standardized TPLO closure protocols commonly include:
- Treating closure as a defined intraoperative phase
- A final lavage step prior to layered closure
- Defined exposure time and sequence
- Immediate saline irrigation before closure
- No change to instrumentation or operative flow
These elements are often already present — standardization simply formalizes their execution. The goal is not to replace surgical judgment — but to reduce unnecessary variability at the final controllable step.
As these elements become formalized, closure protocols increasingly function the same way prep and implant selection do — as defaults rather than case-by-case decisions.
